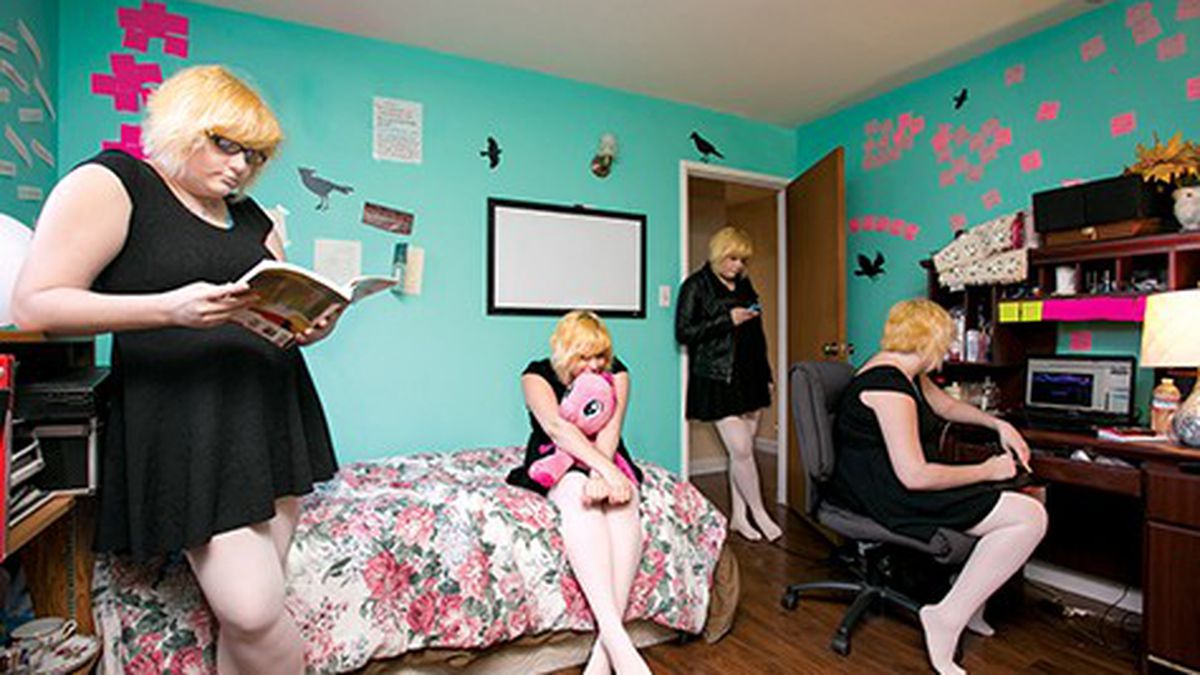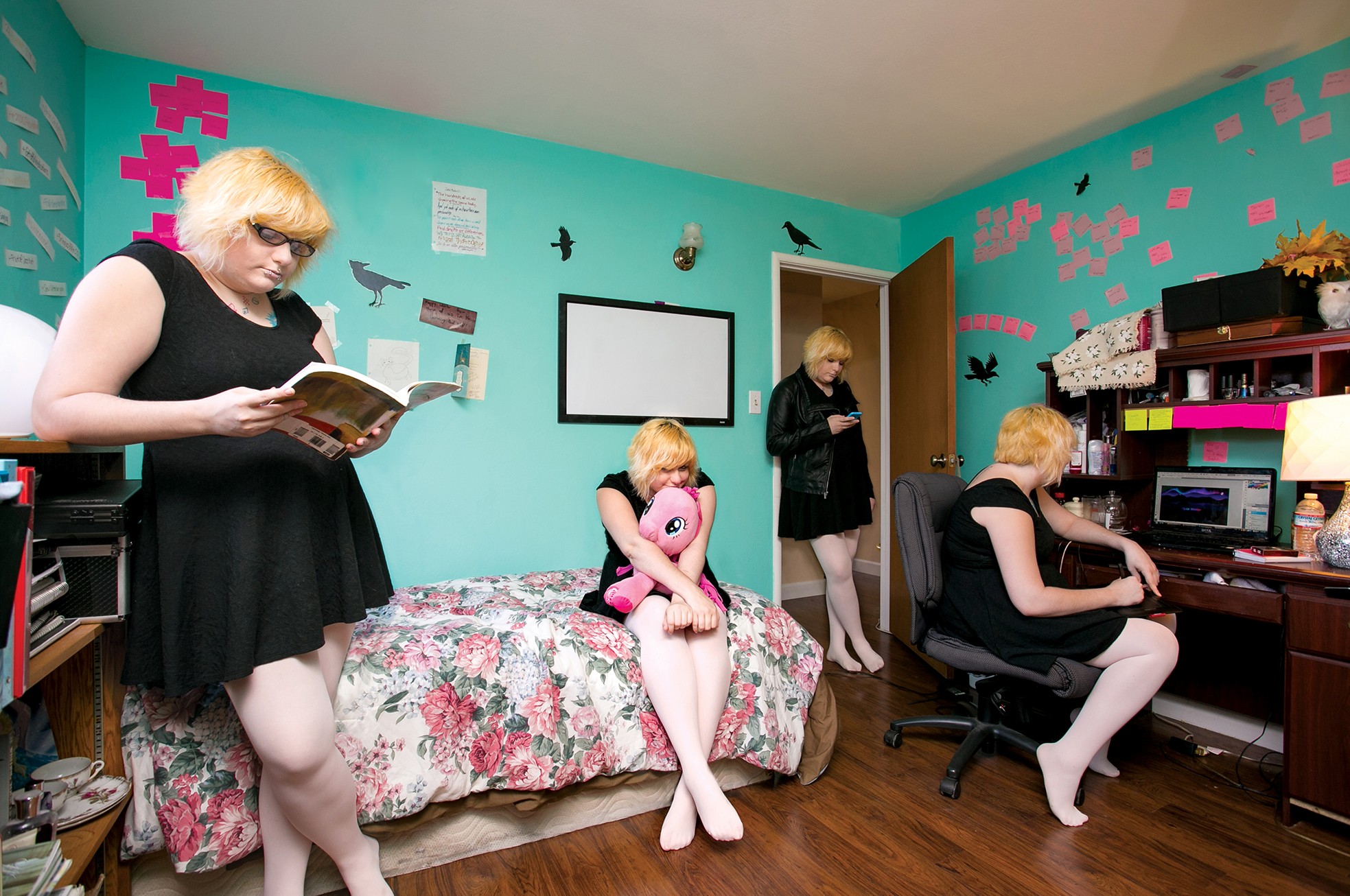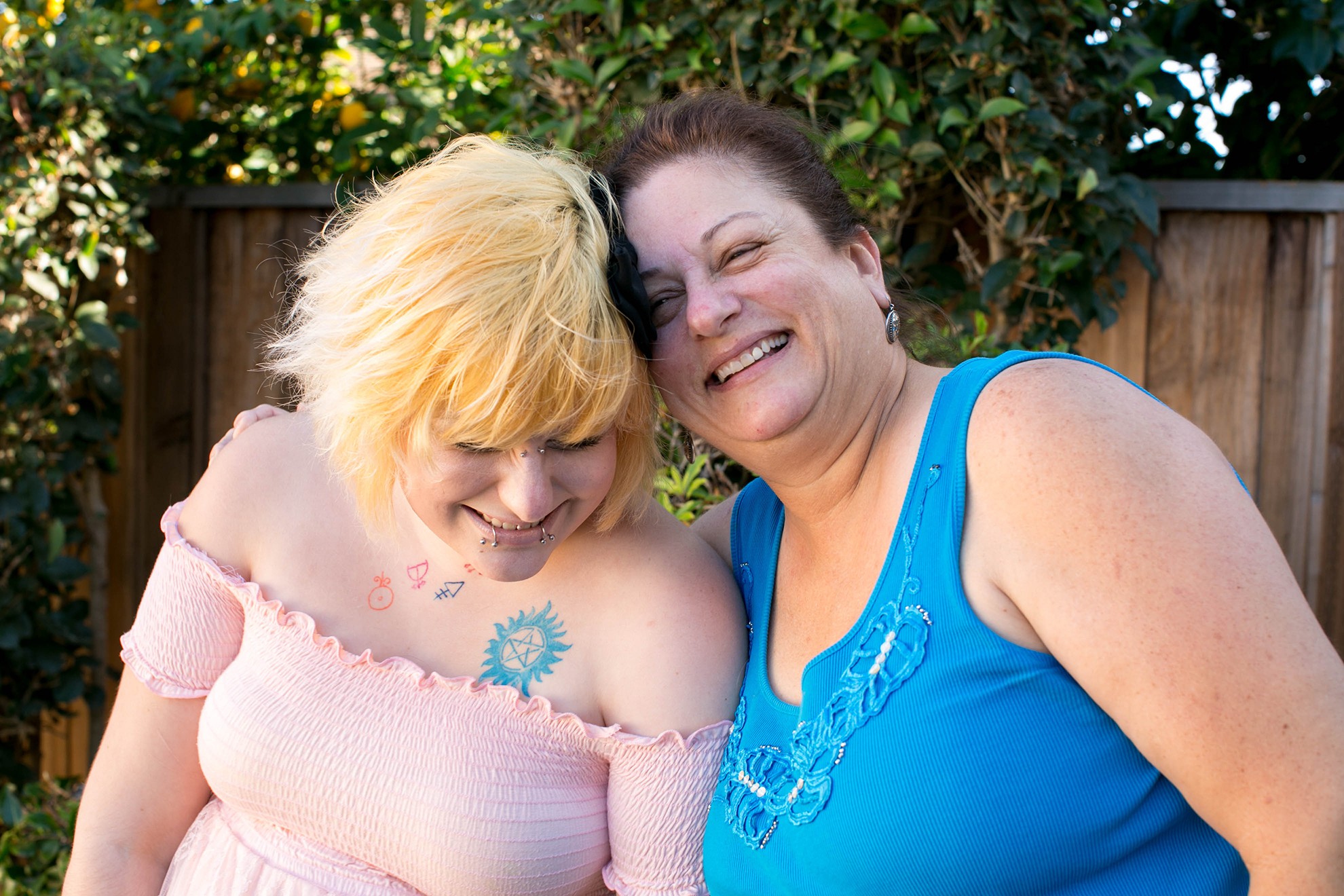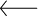At first, the fire trucks sounded distant, but then the blaring horns grew louder. Elyse Winter-Volkova became distressed. It was a sunny afternoon in September, and we were seated at the outdoor patio of a small coffee shop a few blocks away from the San Leandro BART station. It was the first time I had met Elyse, a 21-year-old San Leandro woman, and we had been talking for nearly two hours — about her childhood; her unconditionally supportive mother; her partner, Ben; her struggles in college; her goal of becoming a psychologist; and the tattoos she hoped to get.
When we began our conversation, Elyse was warm and friendly, at times goofy and giggly, immediately talkative, and happy and eager to share stories of her life.


Elyse Winter-Volkova has eight main alters — the term she uses to describe her different identities or personalities. Credits: Photo by Bert Johnson/Illustration by Roxanne Pasibe 
Elyse said her mom, Renee Bergman, has been “very understanding, very accepting.” Credits: Bert Johnson 
Bethany Brand, a professor of psychology at Towson University, recently completed the world’s largest study on the treatment of dissociative disorders. Credits: Kanji Takeno 
Bert Johnson Elyse celebrates her “main eight” with a constellation of post-it notes on the wall above her bed. Credits: Bert Johnson 
Rachel Elise makes paintings, including Face Off (above), about her dissociative disorder. Credits: Courtesy of Rachel Elise 
Credits: Illustration by Roxanne Pasibe 
Then the fire trucks came.
“Oh god,” she said, as the sirens intensified. She turned her head in the direction of the noise, trying to figure out if the emergency vehicles were headed our way. “Where is it? Oh wait, there it is. Ahh, do not turn down here. God!”
Elyse buried her head in her hands on the table. A moment later, the deafeningly loud fire trucks came speeding down our block. Finally, after about ten seconds, the sirens faded into the distance.
“I’m sorry,” I said, awkwardly breaking our silence as she lifted her head from her arms.
She looked irritated and angry and stared at me with a disarmingly cold glare. “It’s not like you control it,” she quipped, before gesturing to herself and saying, “Mae.”
“Mae, hi,” I replied.
“Loud noises are a huge trigger,” she said.
One more loud fire truck sped by. But this time, she didn’t bury her head or even flinch. Mae was unfazed.
At that point in our conversation, I already knew that Elyse suffers from dissociative identity disorder, the condition formerly known as multiple personality disorder. The alarming sound of the sirens had caused Mae — one of Elyse’s main “alters,” the term she uses to describe her different identities or personalities — to take control of her body. In her “system” — meaning her collective group of alters — Mae is the “protector.” That means Mae often comes out when Elyse or any other alter feels threatened or upset.
In fact, shortly before the sirens sounded, Elyse was describing Mae in detail to me while discussing how important it is to her that the people in her life treat each alter with respect. When people are dismissive of her system or her disorder, Mae comes forward, she said.
“Mae will kick their ass,” Elyse joked. “Because she’s like, we deserve respect. … We deserve basic human compassion, you know?”
When the Mind Splits from Bert Johnson on Vimeo.
After the switch, I finished the rest of our conversation with Mae, who has a slightly deeper voice than Elyse and a more sarcastic and dry sense of humor. Mae doesn’t smile often. But she echoed Elyse’s comments about the importance of people accepting her, albeit a bit more directly: “Respect is important,” Mae said. “We’re people and we deserve it. And if anyone doesn’t respect even one alter, they’re in trouble with me.”
I met Elyse a few weeks after she sent me an email, stating that she has was trying to find a journalist to help her raise awareness about dissociative identity disorder, or DID (pronounced D-I-D), a misunderstood and stigmatized condition that is far more common than most people realize. Elyse was officially diagnosed with DID two years ago at Stanford University Medical Center, but she said she has had the condition for much longer.
“The majority of the public knows little to no correct information about DID, and even those in the professional field of psychology debate whether or not this disorder is even real,” Elyse wrote to me over the summer. “But it is. It is very, very real, and so I am working hard to spread awareness.”
Research has increasingly demonstrated that DID is a trauma-based disorder that typically emerges among people who have experienced childhood sexual or physical abuse. Dissociation occurs when people mentally detach themselves from their surroundings, a common coping mechanism for a child victim of abuse. When the abuse continues over a period of time, that dissociation can become extreme and lead the victim to develop distinct, dissociated parts of himself or herself that exist to withstand the abuse.
Experts on DID say that roughly 1 percent of the population suffers from the condition, making it as common as bipolar disorder or schizophrenia. Yet despite this prevalence, the condition remains under-researched and highly controversial, with some psychologists continuing to express doubts about the legitimacy of the disorder.
The result, DID researchers and advocates say, is that victims of trauma can be revictimized by a mental healthcare system that is deeply and unjustifiably skeptical of them. In some cases, sufferers may be misdiagnosed and given treatment and medications that only do more harm. And few therapists are properly educated about the disease.
In the same way that society can be quick to blame rape survivors or assume they are lying, people with DID, who have been victimized in the most unimaginable ways, are also regularly dismissed as fakers and subsequently fail to get the support they need to overcome their traumas. And this struggle is only further exacerbated by deeply ingrained stigmas about mental illness as well as sensationalized stereotypes in film and television, which often portray people with “multiple personalities” or “split personalities” as violent psychopaths.
These are just some of the many reasons why Elyse is speaking up. She openly talks about DID to anyone who will listen and discloses her condition to nearly everyone she meets. She speaks out on Tumblr and YouTube, gives lectures at local psychology classes, and is now trying to draw attention to DID through the media.
Over the course of a series of interviews over the last two months, Elyse and the people closest to her told me about the traumas that led to her DID, what it’s like to live day-to-day with the condition, how her own system of alters has evolved over time, and why it’s critical that people stop dismissing DID as a made-up condition. After all, it’s been her reality most of her life.
Every year, child protective service agencies in the United States receive more than 3 million reports of child abuse. In 2012, there were nearly 63,000 documented cases of child sexual abuse, according to US Department of Health and Human Services data. And experts believe that the number of cases reported and investigated represents just a small fraction of the abuse and trauma that children suffer across the country.
“When they are reported, they are not dealt with well,” said David Spiegel, associate chair of psychiatry and behavioral sciences at Stanford University School of Medicine and an expert on dissociative identity disorder. Some research has suggested that two-thirds of child trauma cases aren’t reported, he said. “These children have to live with it. How do you live with it? … You act as though it isn’t happening or it’s happening to somebody else that isn’t you.”
Cases involving the most severe and disturbing trauma — prolonged physical and sexual abuse by parents, other family members, or caregivers — are especially likely to go unreported. And so children in these cases develop their own ways to survive. “You can’t run away. You can’t fight it, so you go away in your head,” explained Bethany Brand, a clinical psychologist and professor of psychology at Towson University in Maryland, who recently completed the world’s largest study on the treatment of dissociative disorders. “That makes it easier to disconnect from the body in pain.”
When a young mind repeatedly enters these dissociative states in response to ongoing abuse, the coping mechanism can evolve into DID. “It’s an interesting paradox of sort of breaking apart, so that you don’t break,” explained Janelle Salah, a Berkeley-based therapist who treats DID patients.
Someone with full-blown DID will, in response to all kinds of triggers, frequently dissociate into specific parts, or alters, that can become an integral part of that person’s day-to-day life — and can persist after the abuse has stopped.
Brand said that, based on the most comprehensive surveys on the disorder, experts believe that the vast majority of DID patients suffered abuse as children — with some studies suggesting that as many as 90 percent of people with DID experienced sexual or physical abuse during childhood.
A 2006 Journal of Psychiatric Research study concluded that 1.5 percent of the general population has DID. And a 2011 epidemiological overview of DID studies — which stated that “dissociative disorders constitute a hidden and neglected public health problem” — said the disorder exists in 0.4 to 3.1 percent of the general population, and in roughly 5 percent of psychiatric patients. That study also stated that dissociative patients are more likely to report childhood psychological trauma than people suffering from any other psychiatric disorder.
People with DID also are often not diagnosed, experts say. That’s partly because many sufferers also have other mental health disorders related to their abuse — such as posttraumatic stress disorder, anxiety, and depression — which can make DID harder to identify. And as a complex coping mechanism, DID helps people conceal their trauma and pain from the people around them, which can also make it difficult to recognize. (Elyse explained it to me this way: “The main purpose of DID is to hide … and to act as if everything is normal.”)
There’s also a notable lack of research and consensus on DID in the field of psychology. Brand recently did a search for studies on the treatment of dissociative disorders since 1950 and found a total of only 151 research articles — an incredibly small number compared to papers on the treatment of schizophrenia (8,124), bipolar disorder (3,785), and posttraumatic stress disorder (1,236).
It wasn’t until 1980 that the American Psychiatric Association officially added “multiple personality disorder” to the Diagnostic and Statistical Manual of Mental Disorders (DSM), the definitive handbook on mental illnesses. In 1994, the DSM changed the name of the disease to “dissociative identity disorder” and defined the condition as the presence of two or more distinct personality parts or states.
The new name was aimed at presenting the condition as the fragmentation of identity — a failure to integrate different parts of self, explained Spiegel from Stanford, who chaired the group that recommended the change to DID. That fragmentation is fundamentally a problem of memory, he said, meaning some parts of the self don’t remember other parts’ experiences, which can result in temporary amnesia. Some parts may be protecting the “host” — the main alter — from painful memories of abuse.
Despite the disorder’s recognition in the DSM, as well as research demonstrating the distinct brain activity of people with it, DID and the role of trauma in causing it remains controversial among mental health professionals — much to the frustration of those who have studied it extensively and to those living with DID. Some researchers still debate the legitimacy of DID diagnoses and continue to question whether the past trauma that DID patients cite actually happened at all.
But critics say the doubts that some clinicians have about DID only make it harder for victims to come forward and get the help they need to survive.
Elyse realized she was different when she was in second grade. She was born in Banta, a tiny, unincorporated town in San Joaquin County about seventeen miles south of Stockton, and split her childhood between San Joaquin County and San Leandro.
“As a little kid growing up, I thought it was just normal for people to have other people in their heads who took over — that was all I knew,” recalled Elyse, who today has bleached blonde hair, colorful tattoos on her neck and chest, and a number of face piercings.
When her friends role-played at school, she figured that they, too, had other personalities inside of them that were coming out. “When they were pretending to be other people, I actually thought they were other people, because that’s what I was experiencing,” she said. But in elementary school, friends told her it was strange that she would use different names — like Mae — and that’s when she started to grasp that her situation was different.
Elyse said that she is certain now that she has had DID since she was a young child, and that she developed the condition as a way to cope with the extremely severe sexual abuse she suffered over many years. She and her mother, Renee Bergman, who she lives with today in San Leandro, both told me that Elyse, starting at a very young age, experienced repeated physical and sexual abuse by two family members. For years, the two family members molested and raped her frequently and one of them subjected her to intense verbal and psychological abuse, Elyse said. The Express has agreed to not identify the two family members who allegedly abused Elyse because Elyse and Renee said they’re not ready to tell some other members of their family about the specifics of what happened.
Elyse did not tell Renee about the abuse until about two years ago. They both said that for many years, Elyse’s DID helped her conceal the abuse from the people closest to her, including her mother.
When Elyse talked about her childhood, she interchangeably referred to herself in the first and third person, with both singular and plural pronouns. That’s because, as Elyse explained it, the person she is the majority of the time today is not the same person she was for most of her life. Elyse, she said, is currently the “host” of her system, meaning that Elyse is the alter who spends the most time “out” or “fronting” — essentially the one in control of her body. But it wasn’t always that way. For most of her childhood and teenage years, Blue was the host, not Elyse, she said. (Her family considered Blue a nickname and mostly called her by her birth name, Brittany. But she does not use that name now, and plans to legally change her name to Elyse soon).
Elyse recalled that her DID began causing serious problems for her at around age thirteen or fourteen when she started to suffer from periods of distressing memory loss. That is, certain alters would come out, but then when Blue, the host, returned, she would have no memory of what happened when other alters were in control. That became especially problematic when alters would behave badly — for example, by getting in fights with friends, which Blue would not remember the next day.
At one point in high school, Blue lost more than a full day, and when she came to, her computer was open to a page about dissociative identity disorder. Elyse now thinks that one of her other alters was trying to pressure Blue into acknowledging the disorder and to embrace the inner alters.
“I wanted to be normal so bad, but it’s like you’re not normal, dear,” Elyse said. “If it’s not convenient for your traumatized mind to know that you have DID, it’s going to seal it off.”
Eventually, Blue came to terms with DID and started speaking openly about it to some of her close friends, and at age nineteen, about two years ago, she decided to tell her mother about the disorder — and the unconscionable abuse she had experienced as a child.
In all of our interviews, Elyse was the most emotional when recounting how immediately supportive her mother was. “It was a lot to process, but she was, from the get-go, very understanding, very accepting. And I consider myself so lucky for that … because a lot of people don’t have even one parent or one person in their life who is accepting.”
Renee, her 55-year-old mother, recalled the pain of learning about the extreme abuse her daughter had suffered: “It just puts you into a shock. It’s almost like all thoughts leave your head and you don’t even know what to think or feel and you just can’t wrap your head around it.” She didn’t know anything about dissociative disorders at the time, but Renee said she never doubted her daughter.
Soon after Blue told Renee about the abuse, they got an official diagnosis from a Stanford psychologist, which confirmed what they both already knew and provided them with formal documentation, which has been helpful for insurance purposes and doctors’ appointments. Everywhere she goes, Renee carries a letter in her purse from Stanford that references her daughter’s diagnosis, which she showed me on one of my visits to their house on a quiet street in San Leandro.
Renee said she has worked hard to accept her daughter and her alters, who started coming out more regularly after Blue opened up about her DID. When I asked Renee to recall when Elyse took over for Blue as the “host” role in the system, she struggled to find the words. Blue was going through a rough time and she started to disappear, Renee explained.
“Elyse came out, and Elyse kept staying out,” Renee recalled. It was the first time she had met Elyse. At the time, she began to ask Elyse where Blue was, and Elyse would tell her: “She is still hurting. She is on the inside.” After weeks of being gone, Blue finally reappeared — very briefly. At that time, Elyse was in the hospital at Stanford for a very bad migraine and Renee’s mother, sister, and niece were also there for support.
“[Blue] said hello to each one of us. And I just started crying, because I hadn’t seen her. She’s my child. She’s the one I raised, the one I knew,” Renee recalled, in tears. “And she said, ‘Oh mom, don’t be upset.’ She said: ‘I love all of you, and I’m going to go back inside now.'”
Renee paused. “And I’ve never seen her again.”
For Elyse, living with dissociative identity disorder today is very different than what it was when she was younger. For the most part, she doesn’t suffer temporary amnesia anymore, and she said she and her alters can communicate fairly well with each other.
Citing an analogy she learned from a friend with DID that she met through Tumblr, she explained life with DID this way: It’s like her body is a car, and the alter that is “out” is in the driver’s seat. Another alter may be sitting in the front passenger seat, and thus can see, hear, and later remember pretty much everything that is happening. Some may be in the backseat where it’s a bit more blurry. And some may be in the trunk where they can’t see or hear anything.
When she was young and experiencing frequent periods of amnesia, Blue was in the trunk, she explained. But today, she’s developed a more refined system of “co-consciousness,” meaning different alters are essentially present at the same time.
Ben Medina, Elyse’s twenty-year-old partner who has been dating her since March, told me that when he is with her, it’s as if he’s talking to one person, but that person is standing in front of a two-way mirror where many other people — who he cannot see, but who can see him — are watching and are present.
This means there’s a lot of chatter in Elyse’s mind at once, which can lead her to become temporarily distracted mid-conversation. When I talked to Elyse, she would interrupt herself at times to laugh at or point out something that Mae or another alter had just told her. Alters also communicate with each other in more abstract ways, she said, such as by sharing images, thoughts, or feelings.
Different alters will vote on or discuss major decisions that affect the whole body, Elyse said. For example, they all agreed on the words of her back tattoo, which reads, “Taking back what’s mine, one inch at a time,” a message about reclaiming her body from her abusers. (Not all the alters, however, wanted bleached blonde hair, but enough of them supported the idea, she said).
Elyse said she now has eight “main alters,” including herself, who appear regularly, though she said there are many more inside her. There’s Mae, the 25-year-old protector; Jazz, a 24-year-old “fabulously gay” man who has a cockney accent; Nevan, a 25-year-old bisexual male scholar; Candy, a loud teenager; Ophelia, a 22-year-old model, who is also British; Ellie, a four-year-old girl; and Castiel/Gaz, a “gender-fluid” alter — meaning sometimes male, sometimes female, who also fulfills a protector role.
As for her last name, Elyse does not use Brittany’s birth name, Bergman, but rather goes by Winter-Volkova, a combination of the last name that Elyse had before she was host (Winter) and Mae’s last name (Volkova). She calls her whole system the Hydracorn System — Hydra is a reference to the monster in Greek mythology with many heads and the “corn” is a reference to unicorns, which some of the younger alters in her system wanted included in the name.
She generally can’t control which alter is out when — each one comes out in response to certain triggers. When one alter goes back inside, it feels a bit like the moment right before you fall asleep, Elyse explained. And “if you’re on the inside coming out, it’s sort of just like a shock, bam, okay, I’m here. What’s up?” she said.
Every time I met with her, Elyse was out, except twice when Mae came forward — both times in response to certain negative triggers (once when the fire truck sirens blared, and a second time on a different day, when Renee delivered some bad news to her about a sick friend).
Elyse tells pretty much everyone she meets about her DID and her system of alters. Her introductory spiel goes something like this: “I have a disorder called dissociative identity disorder, which used to be known as multiple personality disorder. It’s a real thing.” She then talks about some of the main alters that you might meet and says, “If you don’t know who is out just ask. And if you have any questions, just ask. And if you’re disrespectful, there’s the door.”
Last summer, after she had told many people close to her about her DID, Elyse decided to officially disclose it to all of her friends and family through a Facebook post. She wrote: “So many of you may not know this about me, but I’m ‘coming out’: I have Dissociative Identity Disorder! … I’ve had this mental condition — more a way to cope with what otherwise could have killed me — as long as I can remember.” She asked that people “keep an open mind and not judge before knowing.”
Some were supportive. But others were not. Some relatives stopped talking to her or privately expressed doubt or concern to other family members, Renee and Elyse told me. Elyse had made very clear that people should call her Elyse — and not her birth name — but some refused. “There are a couple family members that just want to sweep it under the carpet,” said Renee.
One family member suggested that because Elyse had taken acting classes in high school, she was fabricating her DID as well as her memories of trauma. “It’s extremely painful for a family member to say something like that,” Renee said.
The problem wasn’t just unsupportive family members. After Elyse began talking openly about DID on Tumblr, she started to face frequent online bullying, often in the form of messages from anonymous users telling her that DID is fake, that her alters are glorified imaginary friends, or that she must be a serial killer.
After she got her diagnosis, Elyse and her mother also had trouble finding therapists with specific expertise on DID. Some clinicians turned Elyse away because they said they didn’t know anything about DID. Renee also recounted having difficulty finding someone at a local rape crisis center to help Elyse; the center said it was trying to connect her to someone with knowledge of DID, but eventually told Renee that there was no DID expert that accepted Elyse’s insurance (Medi-Cal).
One of the worst situations involved a therapist who called Elyse back, shortly after she had received her diagnosis, and told her that the disorder is not real. “I can’t believe a therapist would say something so damaging,” Renee said.
The therapist, Elyse recalled, essentially said: “DID is just made up by the media for insecure people who want attention, and I think you have some seriously deeply ingrained issues if you think that you have all these people in your head.”
According to Brand, the Towson University expert, graduate schools do a poor job of teaching future mental health clinicians about dissociative disorders and the role that trauma plays in psychological conditions. As a result, there are not enough therapists who have the expertise to treat DID. Brand said that in her own practice, there is such a high demand from people with DID seeking psychological services that she has to turn away multiple people every week because her schedule is full.
And because the research on DID is limited, counterproductive debates about fundamental aspects of DID continue today, she said.
These debates have escalated recently over two competing philosophies — the “trauma” and “fantasy” models — concerning dissociative disorders. Arguing in favor of the trauma model, Brand and Spiegel, from Stanford, along with a number of other experts in the field, wrote an article published in Psychological Bulletin in 2012, stating that an abundance of research demonstrates a strong correlation between dissociation and sexual and physical abuse. Many of these studies, the authors noted, have relied on objective, verifiable measures of trauma — meaning confirmations from therapists, reports from child protection agencies, and more.
The second model, which some call the “fantasy model,” suggests that “fantasy overlaps with dissociation” and that people with DID are often prone to fantasies and irrational thoughts and may be vulnerable to suggestive influences from therapists. In other words, this model postulates that therapists may be misleading vulnerable patients into falsely believing that they have other personalities inside of them — and falsely believing that they were abused earlier in their lives. They are prone to “inaccurate or exaggerated self-reports of trauma,” proponents of the fantasy model wrote in a 2014 Psychological Bulletin paper.
“There’s a certain denial about child abuse,” said Spiegel, adding that the argument that people make up their trauma stories are unfounded. In truth, he said, research has demonstrated that trauma victims frequently suppress painful memories of their abuse (which is why they may emerge later in therapy). He pointed to a 1994 study of 129 women who had been sexually abused when they were children, according to hospital medical records. The study found that 38 percent of these women did not recall the abuse. In addition, women who were victimized at a very young age and those who were molested by someone they knew were more likely to have no recollection of the trauma.
The debate about DID is not merely an insider squabble within academia. The fantasy model not only cast doubts on victims of trauma who speak up, Brand said, but lends credence to viewpoints opposing proven methods of treating and supporting DID patients through therapy — therapy that involves engaging alters and working through past traumas.
According to Brand’s recently completed international study on the treatment of dissociative disorders (a broad category that includes DID), psychological therapy produces numerous positive results. It was the first study of its kind: Brand recruited 292 therapists and 280 patients from nineteen countries and tracked their progress over 30 months. She discovered that patients who were in therapy for the longest periods of time experienced the fewest instances of depression, PTSD, and general distress.
Long-term therapy also led to a decrease in the number of suicide attempts, self-inflicted injuries, and hospitalizations. Brand found that 38 percent of patients in the earliest stages of therapy had attempted suicide in the previous year. But those in the most advanced stage of therapy had made no such attempts. And while 40 percent of patients in the first stage of therapy required hospitalization in the year prior to the study, only 5 percent of patients in the advanced stage of therapy needed to be hospitalized.
This research, Brand said, not only demonstrates that people with DID can and should be helped through treatment, but that treatment also has financial implications. Research shows that the cost to treat DID patients nearly doubles if patients aren’t properly diagnosed. It costs an average of $75,000 annually to treat a single person with DID if he or she has not been properly diagnosed, according to Brand. That amount plummets to $39,000, for those who have received accurate DID diagnoses and have begun DID-specific mental health treatment. “These are savings to the individual patient and also to the mental health system,” she said. Those savings primarily come from a reduction in hospitalizations and emergency room visits.
In addition, incorrect diagnoses can have irreversibly harmful impacts for people with DID. For example, if a patient is misdiagnosed as having schizophrenia — a disorder characterized by hallucinations or delusions, an entirely different phenomenon than DID — he or she may be prescribed antipsychotics, which can be very sedating and can have serious side effects, such as permanent facial tics. DID patients misdiagnosed with bipolar disorder may be given lithium, which also carries major side effects.
There are no existing anti-dissociation medications, and experts agree that the disorder cannot be directly treated with prescription drugs, because it’s not associated with a specific chemical imbalance in the brain (which is a factor in schizophrenia and bipolar disorder). Brand said that this is likely one of the reasons that pharmaceutical companies don’t fund studies on DID, which contributes to the illness being under-researched.
Given these factors, Brand and other supporters of the trauma model have become increasingly frustrated with the fantasy model and those who contend that treatment that helps patients cope with past traumas, including talking with alters, is unhelpful or even harmful.
In a recent Psychological Bulletin article that critiqued the trauma model, Steven Jay Lynn, a psychology professor at the State University of New York-Binghamton, along with researchers from six other institutions, including Harvard University, maintained that a variety of stressors “can foster the propensity to fantasize.” Although the researches stated that they were “open to the possibility that trauma may play a nonspecific causal role in dissociation,” their central argument was that the evidence that trauma leads to DID is weak and that the trauma model ignores critical variables like “fantasy proneness” and “suggestibility.”
In an email, Lynn told me there is evidence to suggest that “DID is co-created by patient-therapist interactions.” He also suggested that media representations — most famously in the movies The Three Faces of Eve (1957) and Sybil (1976, starring Sally Field), and more recently in the Showtime television series United States of Tara (2009–11) — have popularized the concept of DID and the role of trauma in leading to split personalities, and may have encouraged more diagnoses. He further stated that he has treated patients who previously experienced “suggestive therapeutic procedures” and “came to believe they had multiple identities,” only to later “disavow their DID diagnosis as they came to appreciate that their self-perceptions were shaped by their treating therapist.”
Lynn told me that critics often incorrectly characterize his position as one that says that people with DID are deliberately faking. He and his colleagues, he said, do not doubt that “some people come to genuinely believe that they house multiple indwelling selves.”
But Lynn and his colleagues remain highly skeptical of the role of trauma in causing dissociation. And they are skeptical of DID patients’ stories of abuse. “Highly dissociative individuals tend to score highly on measures of symptom exaggeration,” he wrote in his email, “raising suspicions about the authenticity of some of these individuals’ memories and symptoms.”
The people closest to Elyse have never doubted that the abuse that she recalls today occurred — nor do they question the legitimacy of her DID. The fact that some psychologists do not take DID seriously and believe that sufferers have exaggerated their stories of abuse makes Elyse visibly angry.
Yet Elyse also contends that DID does not present serious problems for her anymore. On the contrary, she views DID as a mostly positive force that frequently helps her mitigate the harmful impacts of her other mental illnesses, which do get in the way of her life.
Elyse said that as a result of her past abuse, she also suffers from posttraumatic stress disorder, anxiety, depression, insomnia, and other mental health problems. Those conditions create numerous obstacles in her day-to-day life and come with some fairly debilitating symptoms. She also suffers from chronic physical pain, which her mother suspects is a byproduct of her childhood trauma.
It is the panic attacks, night terrors, and anxiety that need to be addressed through therapy — not Elyse’s DID or alters, Renee said. “Watching her go through physical pain and emotional pain, as a mom, it just kills me to see her suffer,” Renee said. “I want to be able to take it away and I can’t.” That’s where Renee hopes that therapy will make a difference for Elyse: “When she gets all that stuff talked out until she can’t talk about it no more — and it may take years, I don’t know — I’m really hoping it’s going to take a lot of that pain away, too.”
Debates about DID models aside, Elyse and her mother’s perspective on her disorder raises a more complex question about therapy and treatment. Can someone lead a functional life with DID? Or is integration — that is, the fusion of different alters into one identity — the only long-term solution? For Elyse and her alters, the answer is clear.
“We’ve never wanted to integrate. … That’s completely not an option for us,” Mae said during one of our interviews. “It would be like killing everyone in your family … and being alone. No one is going to do that. We’re all friends and family in here.”
Elyse said that she, Mae, and the other alters are constantly working toward the best form of “peaceful cohabitation” that they can achieve — that is, effective communication and harmony among all of them.
While the DID therapists I interviewed told me that the central goal of therapy is often integration, many said they also recognized that this is not always possible, and for some, may not be necessary. Integration may be unrealistic for DID patients, because of the chronic and serious stress they endure or the unresolved painful memories they have of their trauma, or because they lack financial resources for long-term treatment, according to the International Society for the Study of Trauma and Dissociation‘s DID treatment guidelines.
“It’s incredibly threatening to a whole system when you begin to ask that system that helped preserve that human to find a new way. It’s kind of an epic battle,” said Salah, the Berkeley-based DID therapist, adding that “at the heart of dissociation is the conflict to know or not to know.” In other words, for some DID patients, moving toward integration or “peaceful cohabitation” often means confronting intensely painful memories that certain alters may have.
And at its core, therapy is really about moving toward greater mental stability and developing and maintaining strong relationships in one’s life. The path to those goals can be very different for each DID patient. Some people’s dissociation or system of alters may prevent them from holding down a steady job due to memory loss, for example. For others, however, having a system of alters may not be an obstacle to everyday living.
Brand said she would not try to force integration on a DID patient — for the same reasons it would be wrong to pressure someone to adopt a certain sexual orientation or gender identity. But she said if she thinks that the merging of parts will help a patient with his or her life — making it easier for that person to develop meaningful friendships or achieve career goals, for example — she will try to help guide the patient toward integration. It’s never easy. She said one of her older patients often tells her, ‘”this is who I have been for forty years. If I lose parts by integrating them, I lose who I am. I lose my friends.'”
Cathy Rose, a 42-year-old Maryland woman living with DID — and a Towson University graduate, who has been a guest speaker for Brand’s classes — told me that her goal is not to be integrated, but rather to be grounded in the present. That means having the different parts of her system working together and not getting stuck in the past. “I’m learning how DID can be healthy … and I can be healthy with it,” she said.
Rose, who works as an analyst at a bank, said her mind is like an orchestra with a lot of different instruments, and she, as a conductor, is trying to direct all instruments to sound harmonious and play the same song.
Rose’s friend, Rachel Elise, another Towson University graduate with DID — who studied fine art and now does paintings about her disorder — said she would eventually like to integrate, but recognizes that it won’t be easy. “I go to a lot of therapy … and it’s just really hard work,” said Elise, 37. One of the challenges, she explained, is that different parts of her hold different memories of the abuse she suffered — and sometimes have very different perspectives on her past — making it difficult to merge them into a single identity.
Elise said she wants to integrate so that she can have more consistency in her relationships and at her job (she works at a nonprofit that raises awareness about trauma and dissociation). And she wants her day-to-day life to improve. It’s still difficult to navigate the wide range of triggers that affect her, she said, and she sometimes struggles in everyday conversations due to the noise in her head.
She said that she respects that integration is not everyone’s goal, but added, “I would like to come back together as much as possible. … I view it more as a blending together. You don’t necessarily lose anything. It’s just in a different shape.”
Elise noted that the struggle of integration is, in a way, a very extreme version of the challenges that most people face when trying to reconcile internal conflicts, such as the simultaneous feelings of love and hate you might have for someone in your life.
“It’s kind of like what every human has to do if they’re trying to be a more conscious person,” she said. “There are probably very few people on earth who know exactly who they are.”
Evidence that Elyse Winter-Volkova is embracing her DID — and has already found a level of peaceful cohabitation — is everywhere in her life. Elyse showed me different possessions and clothes in her bedroom that belong to different alters, including Mae’s leather jacket (which Elyse got Mae for her birthday), stuffed animals and toys for Ellie (the four-year old), art supplies for Jazz (the 24-year-old man), and a cosmetology kit for Ophelia (the 22-year-old model). She celebrates her “main eight” with a constellation of pink post-it notes on the wall above her bed describing each alter.
Elyse’s mother and partner are also highly respectful of each alter and have developed distinct relationships with many of them. In fact, Ben met Jazz before Elyse and is now dating both of them. He also said he views all of the alters as his friends. After I had coffee with Ben and Elyse, it was obvious to me that the two are incredibly close and that Ben is relentlessly supportive of Elyse and open-minded about her condition.
Renee said she enjoys spending time with different alters and buys gifts for specific ones. “I consider all of her alters as my child.” And she said one of the reasons she is most proud of her daughter is that she is paving the way for others with DID to come forward and speak openly — by showing people that there’s no reason to be afraid of the disorder.
Renee also said she is constantly intrigued by her daughter’s DID when it comes to some of the extreme differences between alters — some have unique allergies, skills, voices, and more. “We always hear that the brain is powerful. … I’ve seen it firsthand. I’m amazed every day.”
Elyse hopes to continue to spread positive messages about DID as she gets older. She is now slowly working toward a psychology degree, taking classes at Diablo Valley College in Pleasant Hill and Chabot College in Hayward. Someday, she would like to conduct research on DID in order to better understand the inner workings of complex systems like hers.
And eventually, Elyse said she would also like to help address some of the root causes of DID — by helping survivors of physical and sexual abuse, perhaps by running a shelter for people who have suffered trauma. Victims often have nowhere to turn to escape abuse and no one to help them through the struggle, she said.
After all, many trauma survivors may not have a Mae to protect them.