Here’s Dr. Tony Iton’s prescription for a healthy West Oakland population: Take a good dose of preschool, add a bunch of trees, regular exercises of hope, and call him in the morning. As Alameda County’s director of public health, Iton has been making a name for himself as the health bureaucrat who doesn’t make pronouncements about smoking and jogging and regular check-ups. He’s trying to do away, he says, with “the idea that health equals health care.”
Since he moved up to the director’s chair a year and a half ago, he has used his position as a bully pulpit from which to speak out about the “social determinants” of poor health and chronic illness. Those determinants bring him into far-ranging domains, including housing policy, urban planning, education, and transportation. And while it may seem like a public health director won’t be able to do much about planting trees or increasing funding for public transportation, “not my department” is a rallying cry for Iton, not an excuse for inaction.
According to Iton, there’s a fundamental misunderstanding about how to reverse the climbing rates of chronic illness. “The contribution of poverty, unemployment, poor housing, poor education, those things are much more predictive of length of life and quality of life than individual choices like smoking and eating well and exercise,” he says. Since he understands the deeper problems that are keeping some Alameda County residents from leading long and healthy lives, he sees no choice but to tackle those issues. “What’s the other option?” he asks. “Maintain the status quo? Is that really an option?”
Iton has been in the media spotlight for the past month as a result of the PBS documentary series Unnatural Causes, in which he and some of his like-minded colleagues spell out the many ways in which economic and racial inequities can lead to disease and early death. To capitalize on the PBS moment, Iton also marshaled his staff to produce a report about how these issues play out in Alameda County, and slapped the report on the department’s web site.
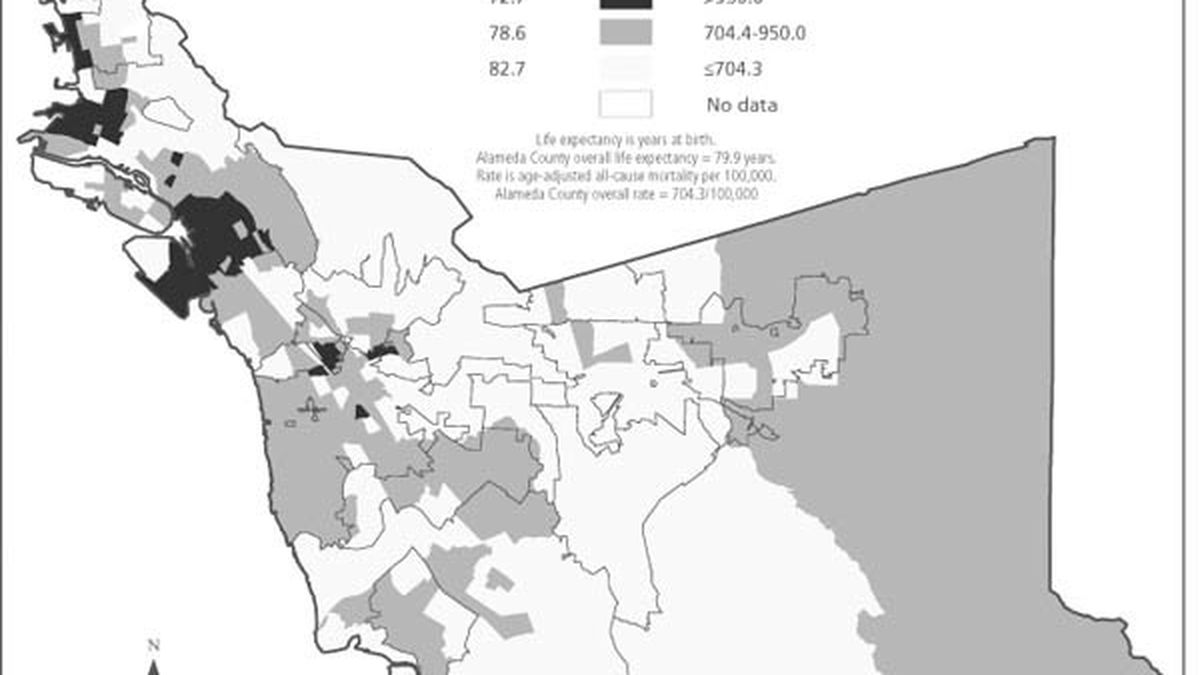
In one startling sidebar, the report shows how life differs for an African-American child born in West Oakland and a white child born in the Oakland Hills. That African-American baby is seven times more likely to be born into poverty, and four times more likely to be born to parents with a high school education or less.
The drumbeat of disadvantages continues — the child will be more likely to be behind in vaccinations, and less likely to read at grade level. Ultimately, as an adult, he will be more likely to suffer from diabetes, heart disease or cancer, and is likely to die almost fifteen years earlier than the white baby born in the Oakland Hills. If that African-American baby wants to have a long, healthy, and productive life, he will have to beat the odds at every step of the way.
Although the report serves as a wake-up call, with harsh statistics drawn from the county’s public health records, Iton says he didn’t want it to be, you know, a big downer. So the report doesn’t just draw attention to Alameda County’s disparities; it also creates an ambitious wish list of policy recommendations. Iton then sent those proposals to his numerous contacts in local government and the nonprofit world, and asked for help in making them a reality.
But when Iton starts talking about cross-cutting initiatives, it can give a cynical listener the vague, worried feeling that he’s talking about holding a lot of inter-departmental meetings. How about an example of how this could work?
Take something simple like high school graduation rates in Alameda County, Iton suggests, where dropout rates are much higher for African-American and Latino students. “If we know that has profound health implications, and also implications in terms of crime, and productivity, and employment, and mental health and stress, then shouldn’t we be making a concerted effort to address the root cause?” he asks.
Iton cites the public health department’s support of Oakland’s Youth UpRising, an after-school center, as an example of an unconventional tactic that might chip away at those problematic dropout rates. “You can ask the public health system just to throw open the emergency room doors, and treat people for heart attacks and strokes and stress and lives of despair,” he says. “Or we can move upstream and look at the determinants of these outcomes that are extremely expensive and are bankrupting our system.”
The busy director has many other plans for collaboration across departments, and also wants to distribute the “Unnatural Causes” report to community groups; he hopes they can bolster their arguments about, say, how to redevelop an old piece of industrial land with statistics about the health outcomes of a park versus a high-rise.
The idea that a baseball field is better for a community than luxury condos is not exactly breaking news, but that’s one of Iton’s gifts: He makes sad old stories sound fresh and urgent. And like a certain presidential candidate, he gives people the feeling that they might actually be able to do something about the problems they face. “Americans feel helpless about things they shouldn’t feel helpless about,” says the Canadian-born Iton. “I don’t think this is hard at all.”